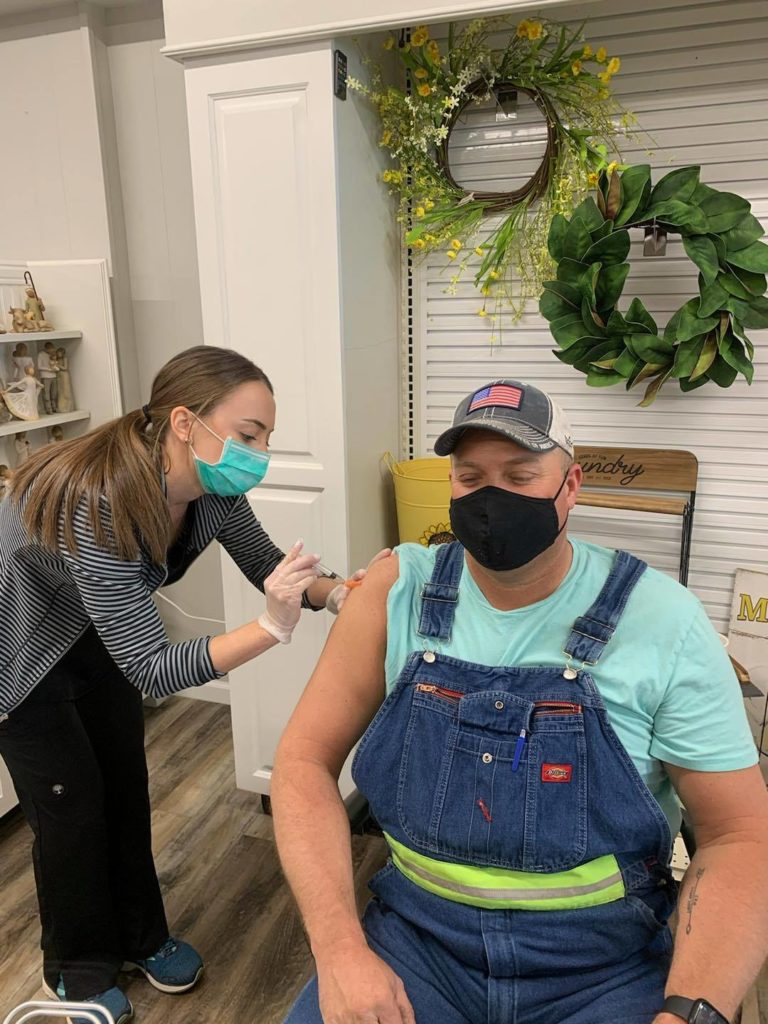

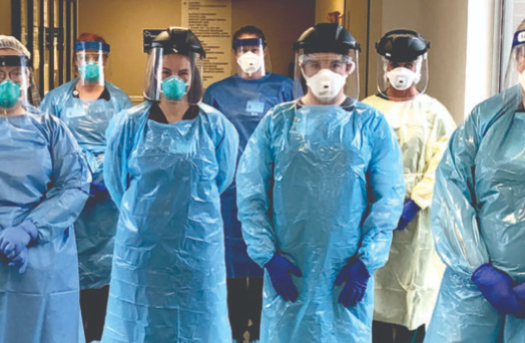
Impacts on Healthcare
Elective procedures stopped on March 18, 2020, to limit traffic in hospitals. This measure allowed to free up healthcare workers to treat COVID-19 patients. Throughout the pandemic, Owensboro Health Regional Hospital (OHRH) took in patients from around the region. OHRH created negative pressure rooms to prevent transmission of COVID-19 into the hallways.
During the pandemic, some people avoided their doctors for regular appointments and non- emergency health issues for fear of being exposed to the virus. Hospitals typically allowed one guest for all doctor appointments, disregarding the severity of the patient’s condition. At times, no guests were allowed. Going to the doctor became even more stressful than usual. Visitors were not allowed for COVID-19 patients. Their only human interaction was with healthcare workers dressed in head-to-toe PPE. Studies already show that COVID-19 patients who spend time in intensive care come home with mental health issues, some even showing evidence of post-traumatic stress disorder.1
Telehealth
Many doctors conducted telehealth appointments to reduce exposure to COVID-19. Telehealth was not unheard of before the pandemic but was not widely used. In the last week of March 2020, there was a 154% increase in telehealth visits compared with the same week in 2019.2 While telehealth appointments can be conducted over the phone, internet access is often preferred so a doctor can see the patient. Telehealth appointments include the benefit of avoiding the hospital and reducing the chances of exposure to COVID-19. Telehealth accessibility is a problem in the GRADD region where broadband is either unreliable or unavailable. Patients who cannot receive telehealth due to a lack of broadband must risk exposure to see a doctor or forego care altogether.
Financial Impact
Owensboro Health Regional Hospital, the largest employer in the region with about 5,000 employees, did not lay off or furlough a single employee despite the challenges. During the pandemic, a state mandate postponed non-emergency medical services. In response, employees working in those departments were reassigned to other departments still providing services. Despite the 65 percent revenue cut the pandemic brought to Owensboro Health, every employee remained on the payroll. Much of that revenue loss was recovered in between surges of the virus, when more non-emergency services were able to resume.
CARES Act funding also played a crucial role in many hospitals continuing payroll and recovering lost revenue. Ohio County Hospital received a share of $3.88 million from the CARES Act, along with 45 other rural hospitals. These funds allowed for the purchase of PPE and testing and laboratory services.
Kentucky Vaccine Timeline

March 2020 brought troubled times when the first case of COVID-19 was identified in Kentucky. Months of uncertainty followed as people questioned their health and pondered whether a vaccine would be possible and when it would be distributed. On December 14th, 2020, Kentuckians received their answer when the first shipment of vaccines arrived in Louisville. That shipment contained 12,675 vials. The first Kentuckians to receive a vaccine were frontline healthcare workers at the University of Louisville Hospital.
The closest hospital to the GRADD region to receive early doses of the vaccine was the Medical Center, in Bowling Green. In February 2021, Ohio County Healthcare became the first facility in the GRADD region to be designated as a regional vaccine distribution site. Additional hospitals, clinics, pharmacies, drive-thru sites, and pop-up vaccination sites opened as the weeks passed.
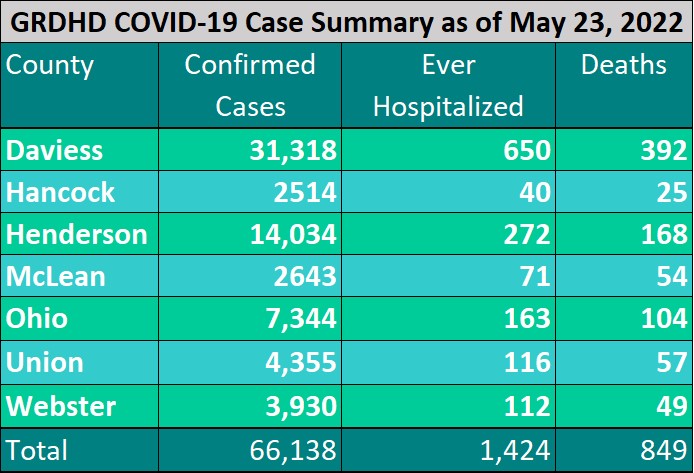
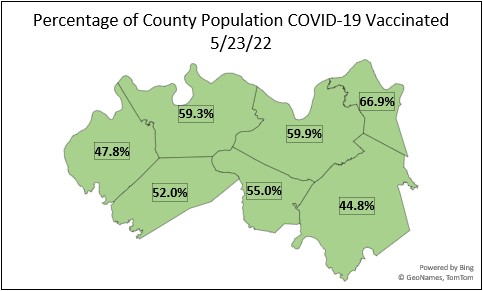
http://healthdepartment.org/news-events/covid-19-press-release/
